High-Speed Dental Lab Scanners in 2025: YRC RS600 & RS1000 Specs for Implant and Ortho Workflows
2025-11-24
2026-03-29
In 2026, zirconia dental implants have emerged as a game-changing all-ceramic option for the maxillary and mandibular anterior zones, where esthetics, soft-tissue harmony, and long-term predictability are paramount. Unlike traditional titanium, zirconia’s tooth-like white color eliminates gray shadowing through thin gingival biotypes, delivering superior pink and white esthetic scores while maintaining high biocompatibility and low bacterial adhesion. Recent long-term data confirm survival rates rivaling titanium in carefully selected cases, with monolithic zirconia restorations simplifying workflows and reducing complications. This evidence-based guide synthesizes 2025–2026 clinical studies to outline breakthroughs, case selection, and protocols for optimal outcomes in the esthetic zone.
Zirconia implants—primarily one-piece or two-piece yttria-stabilized tetragonal zirconia polycrystal (Y-TZP)—offer metal-free solutions that address patient demands for natural-looking restorations. Advances in surface modification (sandblasted and acid-etched ZLA surfaces) and CAD/CAM monolithic designs have narrowed the historical gap in osseointegration and mechanical performance, making them ideal for high-smile-line patients, thin biotypes, and those with metal sensitivities.
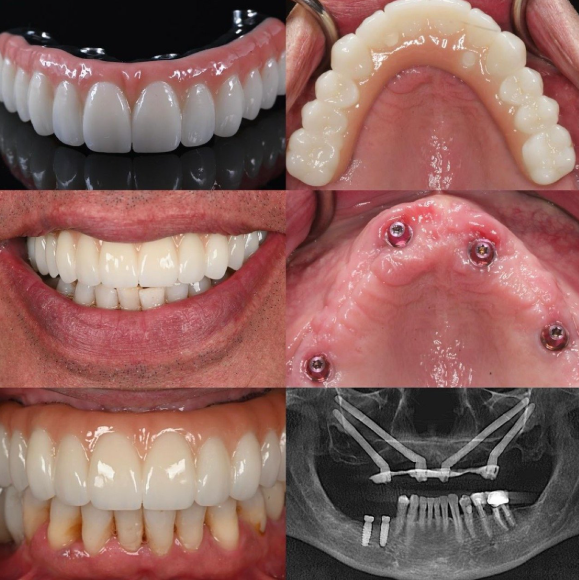
Modern zirconia implants feature optimized micro-rough surfaces that promote osseointegration comparable to titanium in short- to medium-term studies. Flexural strength exceeds 900 MPa, while the white hue ensures excellent light transmission and fluorescence matching natural dentin-enamel. Monolithic zirconia crowns or abutments eliminate veneering chipping risks, with high-translucency formulations now rivaling lithium disilicate in anterior esthetics.
Clinical advantages in the esthetic zone include:
Recent prospective and multicenter studies provide robust data:
Subgroup analysis confirms zirconia excels in anterior esthetics: higher PES scores and zero metal visibility even with minor recession. While some studies note slightly lower overall survival than titanium in high-load scenarios, strict case selection and late placement protocols yield titanium-comparable results in the esthetic zone.
Complications remain low: no implant fractures in multiple long-term series, rare mechanical issues with monolithic designs, and favorable patient-reported outcomes (VAS esthetics 8.6+).
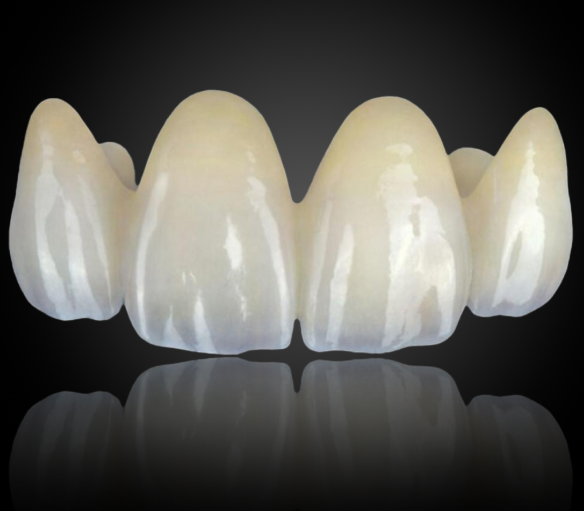
Primary Indications in the Aesthetic Zone:
Contraindications & Risk Mitigation:
Digital Workflow Optimization: Intraoral scans, AI-assisted planning, and 3D-printed surgical guides ensure precise subcrestal positioning. Monolithic zirconia crowns (screw-retained or bonded to Ti-base hybrids where needed) streamline delivery with same-day or short-lab turnaround.
Special Considerations:
Patient factors—age, occlusion, smoking status, and compliance—guide final decisions. Comprehensive digital smile design and mock-ups enhance predictability.
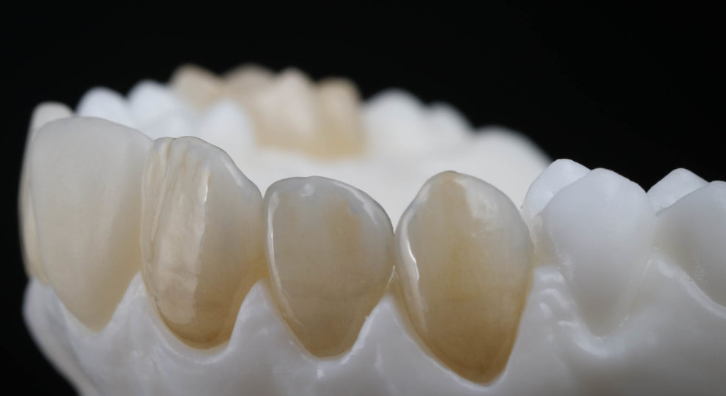
Placement: Flap or flapless with torque-controlled insertion. Subcrestal positioning of the rough-smooth transition in esthetic zones. GBR with bone substitutes and membranes when buccal bone is thin.
Restoration: Monolithic high-translucency zirconia crowns—screw-retained for retrievability or cement-retained on zirconia/titanium bases. Adhesive protocols (MDP primers) ensure retention. Occlusal adjustment via digital analysis prevents overload.
Maintenance: Annual professional cleaning, nightguards for parafunctional patients, and radiographic monitoring at 1, 3, 5, and 10 years. Probing depths typically stabilize at 2.7–3.0 mm with minimal bleeding on probing.
These protocols, combined with 2026 material refinements, yield >95% survival in anterior applications when indications are matched.
Patients consistently rate zirconia implants highly for natural appearance and comfort. In 2026 immediate-therapy studies, overall satisfaction reached 94.99%, with significant improvements in quality of life, speech, and self-confidence. The absence of metal visibility boosts psychosocial acceptance, particularly in high-esthetic-demand demographics.
High-translucency graded zirconia, faster sintering protocols, and hybrid two-piece systems with tissue-level platforms continue to evolve. AI-driven patient-specific designs and bioactive surface enhancements promise even better integration. While titanium remains the gold standard for posterior high-load cases, zirconia’s all-ceramic profile cements its role as the breakthrough solution for anterior esthetics.
Zirconia implants in the aesthetic zone represent a 2026 paradigm shift toward fully ceramic, patient-centered implantology. With 10-year survival rates up to 97.7%, stable bone levels, superior esthetics, and high patient satisfaction, they deliver predictable, metal-free solutions where natural harmony matters most. By aligning material properties with case-specific demands—thin biotypes, high smile lines, and esthetic priorities—clinicians achieve outcomes that rival or exceed traditional options while future-proofing practices.

Dry & wet milling for zirconia, PMMA, wax with auto tool changer.
learn more
High-precision 3D scanning, AI calibration, full-arch accuracy.
learn more
40-min full sintering with 57% incisal translucency and 1050 MPa strength.
learn more

40-min cycle for 60 crowns, dual-layer crucible and 200°C/min heating.
learn more
High-speed LCD printer for guides, temporaries, models with 8K resolution.
learn more