Why Maintenance & Troubleshooting Are Critical for CAD/CAM Dental Equipment in 2026
2026-04-09
2026-04-27
3D printing has revolutionized dental laboratories by enabling rapid production of diagnostic models, working models, surgical guides, and aligner thermoforming bases. Yet many labs face persistent model deviations that result in poor seating, increased chairside adjustments, higher remake rates, and eroded clinician trust. Reconstructing the entire workflow—from file preparation to post-processing—is the most effective way to move from frequent inaccuracies to stable, repeatable production.
Recent studies report root mean square (RMS) deviations for 3D printed full-arch dental models typically ranging from approximately 73 μm to 194 μm, with many falling between 109 μm and 140 μm depending on resin, printer technology (SLA, DLP, or LCD), and process parameters. While these values often remain within broadly accepted clinical thresholds (commonly under 200–250 μm for many prosthetic applications), variability across batches, operators, and environmental conditions drives inconsistency.
Posterior regions and highly curved areas tend to show larger local deviations. Factors such as resin type, layer thickness (50 μm vs. 100 μm), print orientation, and post-processing significantly influence trueness and precision. One study found water-washable resins achieved lower mean RMS deviation (around 109 μm) compared to other formulations, highlighting material impact.
Common failure modes include warping, layer delamination, support failures, dimensional drift, and uneven curing—issues that increase remake frequency and material waste.
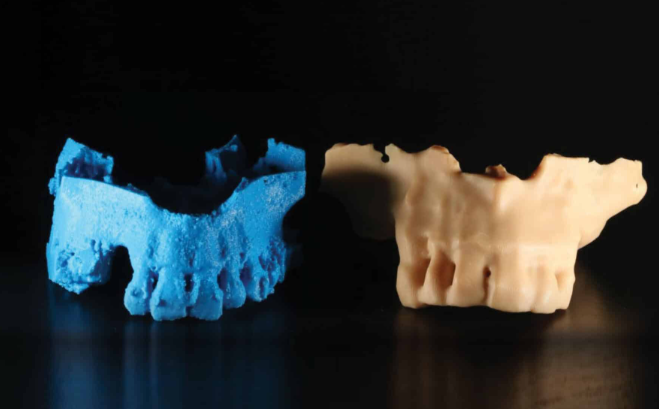
Most deviations stem from controllable variables rather than the technology itself:
Print orientation plays a notable role: extreme angles (0° or 90°) often increase deviations due to support requirements and gravitational effects, while moderate angles frequently perform better for specific features.
Successful labs treat 3D printing as a controlled manufacturing process rather than an ad-hoc operation. Here is a practical reconstruction path:
1. Establish Rigorous Equipment Calibration and Maintenance
Implement daily or shift-based checklists:
Consistent calibration dramatically reduces adhesion failures and dimensional drift.
2. Standardize File Preparation and Pre-Print Validation
Standardized pre-print checks can catch many issues upstream.
3. Optimize Printing Parameters with Data-Driven Settings
Develop resin-specific and model-specific parameter sheets covering:
Regularly print and scan test models against digital references using metrology or superimposition software to quantify trueness (RMS deviation) and precision (repeatability). Adjust scaling factors to compensate for known material shrinkage.
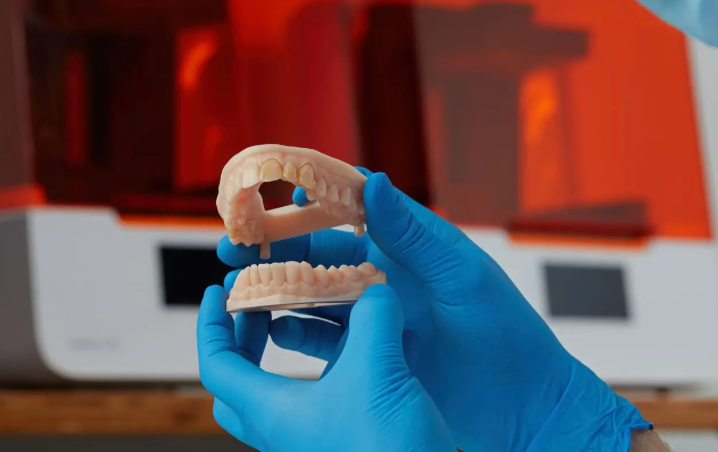
4. Standardize Post-Processing Protocols
Post-processing is frequently the largest source of variability:
Proper, repeatable post-curing ensures dimensional stability, mechanical properties, and biocompatibility. Automated systems can significantly improve consistency over manual methods.
5. Implement End-to-End Standardized Operating Procedures (SOPs) and Quality Control
Labs adopting full standardization often report more predictable outcomes, fewer clinical adjustments, and improved profitability through reduced waste.
Define clinically relevant targets. Many applications tolerate overall deviations under 150–200 μm, though tighter tolerances apply for implant components or high-precision prosthetics. Use RMS values combined with color deviation maps for comprehensive evaluation.
Start implementation with high-volume items like diagnostic or study models, then expand to more demanding applications such as surgical guides. Conduct regular internal audits and continuous training. Over time, data-driven adjustments compound into stable production.
Digital workflows paired with disciplined 3D printing can also contribute to lower overall remake rates compared to traditional analog processes, though exact gains depend on execution.
Frequent 3D printed dental model deviations are not an inevitable drawback of the technology—they are symptoms of inconsistent processes. By systematically rebuilding the workflow around calibration, standardization, validated parameters, and robust quality control, dental laboratories can achieve stable, repeatable production that meets clinical demands.
The result is fewer remakes, faster turnaround, better clinician satisfaction, and a stronger competitive position in digital dentistry. Consistency comes from process discipline, not just better printers or resins. Labs that commit to this reconstruction path transform 3D printing from a variable bottleneck into a reliable manufacturing advantage.

Dry & wet milling for zirconia, PMMA, wax with auto tool changer.
learn more
High-precision 3D scanning, AI calibration, full-arch accuracy.
learn more
40-min full sintering with 57% incisal translucency and 1050 MPa strength.
learn more

40-min cycle for 60 crowns, dual-layer crucible and 200°C/min heating.
learn more
High-speed LCD printer for guides, temporaries, models with 8K resolution.
learn more
2026-04-09
2026-01-19

2025-11-29