The Importance of Technical Support from Denture Processing Labs for Dental Clinics Fostering Collaboration and Communication
2025-04-02
2026-03-18
Dental glass ceramics, particularly lithium disilicate and feldspathic systems, remain favorites for aesthetic restorations thanks to their exceptional translucency, natural light transmission, and etchable surfaces that enable strong adhesive bonding. With high survival rates for single crowns (often 95–97% at 5–10 years), they support minimally invasive preparations in anterior and premolar regions. Yet, inherent material limitations and real-world clinical frustrations continue to restrict their use in high-load posterior applications and multi-unit bridges.
This article details current technical hurdles in glass-ceramic development and the practical issues dentists and technicians encounter daily. Backed by recent clinical and in-vitro data, it equips practices with the knowledge to optimize material selection and workflows in 2026 and beyond.
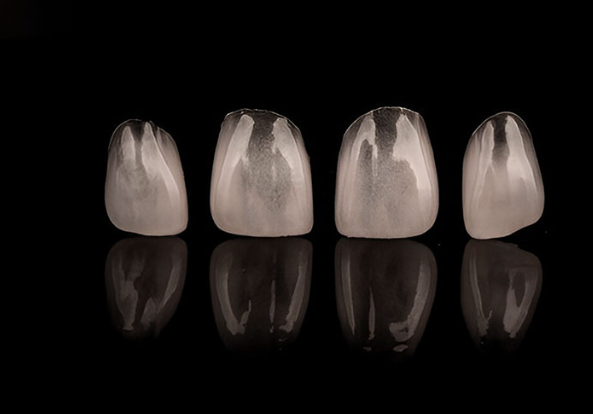
Glass ceramics achieve their unique properties through controlled crystallization of a glassy matrix, but this process creates fundamental trade-offs.
Low Fracture Toughness and Brittleness Flexural strength typically ranges 360–500 MPa for lithium disilicate—far below zirconia's 700–1,100 MPa. This limits indications for posterior bridges and high-occlusal-load cases. Systematic reviews confirm higher fracture risk in molars (5-year rate 8.1% vs. 3.0% in premolars), with overall all-ceramic crown fracture at 4.4%. The glassy phase provides excellent aesthetics but promotes crack propagation under stress.
Chipping in Bilayer Systems Veneered restorations suffer from thermal expansion mismatch between core and veneer, leading to cohesive chipping. Clinical data show veneer chipping as the primary failure mode in layered systems, especially posteriorly. Monolithic designs reduce this dramatically, yet many anterior cases still require layering for ultimate translucency—creating an ongoing strength-aesthetics compromise.
Crystallization Shrinkage and Processing Limitations Heat treatment (typically 840–850°C for lithium disilicate) induces ~0.2% shrinkage in CAD/CAM blocks, but improper furnace cycles cause distortion or incomplete crystallization. Pressed systems demand precise lost-wax techniques, while additive manufacturing introduces porosity, layer anisotropy, and lower density—issues still under active research in 2025–2026. These factors complicate same-day workflows and increase remake risk.
Bonding and Surface Sensitivity Although HF-etchable for excellent micromechanical retention, the process is technique-sensitive. Over-etching or contamination reduces bond strength, and chairside adjustments (grinding) increase surface roughness, lowering flexural strength by up to 20–30% in studies.
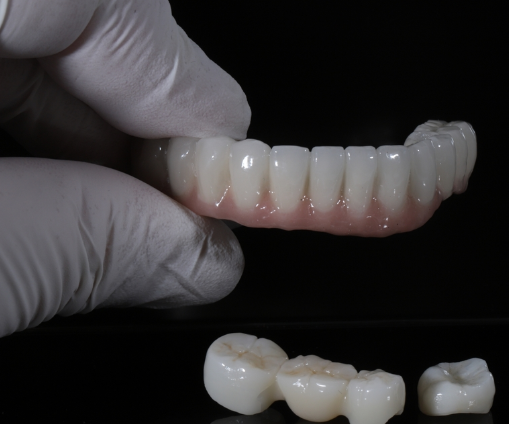
Dentists and lab technicians report recurring frustrations that directly affect longevity and patient satisfaction.
Fracture and Chipping Leading to Remakes Posterior lithium disilicate crowns show higher non-repairable failure rates than anterior ones. Users frequently cite occlusal chipping or bulk fracture in bruxers or unfavorable occlusion, forcing full replacement. Feldspathic veneers exhibit even higher chipping (majority of failures in adolescent trauma studies).
Fit and Adjustment Problems Milling precrystallized blocks or post-crystallization grinding creates microcracks and roughness. Chairside adjustments for marginal fit or occlusion compromise strength and increase wear on opposing enamel. Laboratory crystallization can also cause minor distortions requiring extra polishing time.
Polishing and Surface Finish Challenges Fully crystallized materials are harder to polish than precrystallized states. Inadequate polishing leads to plaque accumulation, staining, or accelerated opposing-tooth wear. Users demand simpler protocols for achieving Ra <0.2 µm consistently.
Limited Indications and Workflow Inefficiencies Many clinicians avoid glass ceramics for posterior bridges or long-span restorations due to fracture risk, defaulting to zirconia and losing the aesthetic advantage. Pressing or CAD/CAM crystallization adds lab steps, delaying same-day delivery compared to monolithic zirconia.
Aesthetic Longevity Concerns Although initially superior in translucency, minor chipping exposes the core or requires repairs that alter shade match over time.
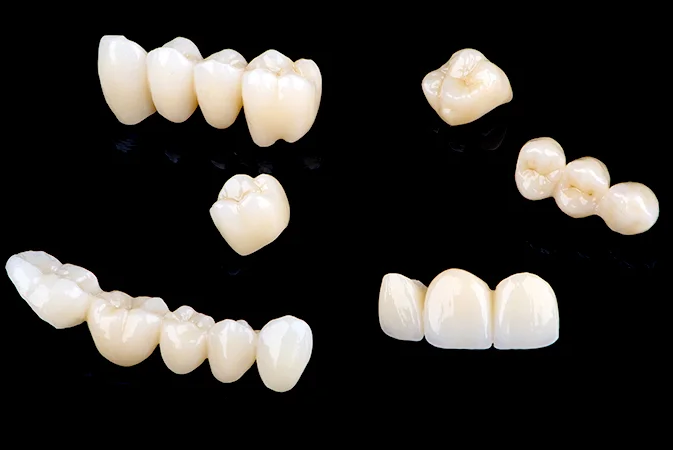
To minimize risks today:
Ongoing advances—nanostructured fillers, improved pressable systems, faster crystallization protocols, and hybrid glass-zirconia formulations—promise higher toughness without sacrificing aesthetics. Additive manufacturing refinements (reduced porosity, better sintering) are expected to expand indications by 2026–2030.
Dental glass ceramics deliver unmatched aesthetics and adhesive potential, yet brittleness, chipping risk, crystallization sensitivities, and processing limitations continue to challenge developers and clinicians. Dentists consistently call for stronger monolithic options, simpler workflows, and more forgiving bonding protocols.
By understanding these constraints and applying evidence-based techniques, practices can maximize success rates while minimizing remakes and patient dissatisfaction.

Dry & wet milling for zirconia, PMMA, wax with auto tool changer.
learn more
High-precision 3D scanning, AI calibration, full-arch accuracy.
learn more
40-min full sintering with 57% incisal translucency and 1050 MPa strength.
learn more

40-min cycle for 60 crowns, dual-layer crucible and 200°C/min heating.
learn more
High-speed LCD printer for guides, temporaries, models with 8K resolution.
learn more