High-Speed Desktop Scanner Adoption in Eastern Europe: Balancing Speed and Precision in Dental Labs
2026-01-29
2026-03-17
Ceramic resin liquids—hybrid composites filled with ceramic particles for 3D printing—have opened new possibilities in additive dentistry, enabling fast, customizable crowns, bridges, and temporary restorations directly at chairside or in labs. With growing adoption in digital workflows, these materials promise efficiency and aesthetics without traditional milling waste. Yet, despite advances, significant technical limitations and practical user issues persist, restricting their use primarily to provisional or low-stress applications.
This article examines current development hurdles in ceramic resin liquids and the everyday frustrations reported by dentists and technicians. Backed by recent in-vitro and clinical data, it helps practices make informed choices while highlighting areas needing urgent improvement.
These light-curable resins combine polymer matrices with ceramic fillers for improved strength and aesthetics, but inherent material science trade-offs remain unresolved.
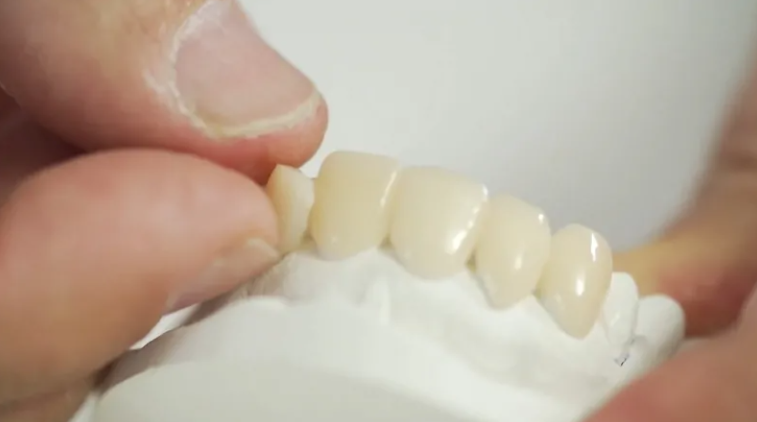
Polymerization Shrinkage and Dimensional Accuracy Volumetric shrinkage during curing (typically 1–6% in resin composites) creates internal stresses, leading to marginal gaps, distortion, and poor fit. Layer-by-layer printing introduces anisotropy—directional weaknesses where interlayer bonding is inferior to intra-layer strength. Recent studies show trueness variations across occlusal, axial, and marginal areas, with some printed crowns exhibiting higher deviations than milled alternatives. Environmental factors like build orientation and post-curing temperature exacerbate shrinkage, causing clinically unacceptable gaps in complex geometries.
Wear Resistance and Mechanical Strength Limitations Ceramic-filled resins underperform traditional ceramics under occlusal load. In-vitro wear testing reveals significantly higher material loss: 58 ± 3 µm for 3D-printed resin crowns versus 25 ± 2 µm for CAD/CAM ceramics (p < 0.001). Clinical follow-ups report occlusal height loss up to 1.25 mm in molars after 24 months, with 35% of restorations showing >0.5 mm wear classified as fractured. Lower filler content and polymerization effects reduce flexural strength and surface hardness, accelerating degradation in high-stress zones.
Post-Processing Dependencies Washing (IPA or alternatives) and UV post-curing critically affect final properties. Over-washing plasticizes the surface, increasing brittleness; insufficient curing leaves residual monomers. Curing temperature influences accuracy—higher heat can cause distortion or shrinkage—while optimal conditions (e.g., 40°C for 15–40 min) are material-specific and hard to standardize. These steps add time, variability, and risk of incomplete polymerization.
Biocompatibility and Long-Term Stability Residual monomers from incomplete conversion pose cytotoxicity risks, with potential pulp irritation or allergic reactions. Water sorption and solubility remain high, promoting discoloration, staining, and mechanical weakening over time. Color stability is a major weakness—printed resins often shift under UV or oral conditions. Occupational hazards include VOC emissions during printing, raising respiratory and skin concerns in clinics.
Material Homogeneity and Printability Ceramic fillers settle in the vat without agitation, causing inconsistent layers and weak restorations. Viscosity challenges limit high filler loading, capping mechanical gains while maintaining printability.
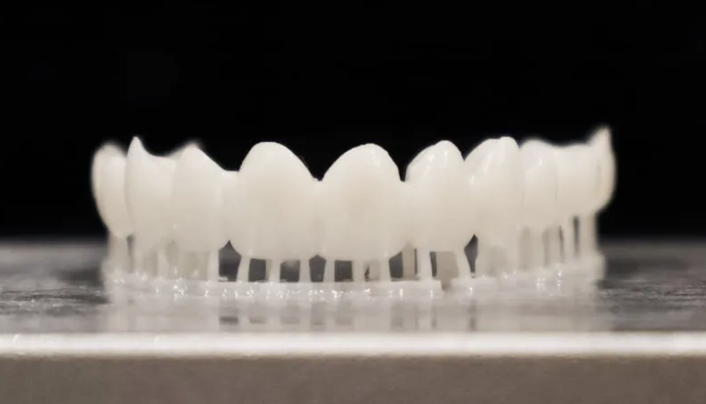
Dentists and lab technicians frequently cite workflow and performance frustrations that impact clinical reliability.
Wear, Fracture, and Remakes Rapid occlusal wear and chipping force frequent adjustments or full remakes, especially in posterior or full-coverage cases. Users report higher failure rates in load-bearing areas compared to milled ceramics, limiting confidence for definitive restorations.
Fit and Adjustment Problems Shrinkage-induced inaccuracies require extensive chairside grinding, risking microcracks or overheating. Marginal adaptation varies, increasing cement failure risk and secondary caries potential.
Post-Processing Complexity Time-consuming washing, drying, and curing steps disrupt same-day workflows. Incorrect protocols lead to brittle parts, monomer release, or color shifts—common complaints in busy practices.
Color and Aesthetic Instability Even multilayer or shaded resins discolor faster than expected, frustrating anterior cases where patients expect long-term match.
Safety and Maintenance Demands Residual monomer concerns and VOC exposure require strict ventilation and PPE. Printer calibration, resin mixing, and tray replacement add ongoing maintenance burdens.

To reduce risks today:
By 2026–2030, expect nanostructured fillers, low-shrink monomers, AI-optimized post-processing, and improved permanent-grade resins with better wear resistance and color stability. Hybrid workflows combining printing with milling will bridge current gaps.
Ceramic resin liquids deliver unmatched customization and speed for 3D-printed restorations, yet polymerization shrinkage, inferior wear resistance, post-processing sensitivities, and biocompatibility hurdles continue to challenge developers and users. Dentists consistently demand stronger, more stable materials with simpler workflows and proven long-term performance.
By understanding these limitations and adopting rigorous protocols, practices can safely leverage the technology while minimizing remakes and patient dissatisfaction. The future of additive dentistry is promising—but informed, cautious adoption remains essential in 2026 and beyond.

Dry & wet milling for zirconia, PMMA, wax with auto tool changer.
learn more
High-precision 3D scanning, AI calibration, full-arch accuracy.
learn more
40-min full sintering with 57% incisal translucency and 1050 MPa strength.
learn more

40-min cycle for 60 crowns, dual-layer crucible and 200°C/min heating.
learn more
High-speed LCD printer for guides, temporaries, models with 8K resolution.
learn more
2026-01-29
2025-09-01
2026-01-31